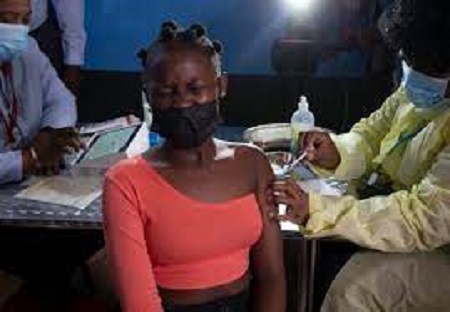
In the early days of the epidemic, South African health officials expected a spike in HIV-related deaths. According to epidemiologist Salim Abdool Karim, who runs the AIDS centre where KRISP is situated, “we were basically constructing horror scenarios that indicated Africa will be decimated.” “But none of it worked.” The fundamental explanation is that H.I.V. affects young individuals whereas the coronavirus affects the elderly.
Some months ago, a clinic alerted Sizakele Mathe, a community health worker in this huge hillside slum on the outskirts of Durban. It was a clue she had stopped taking her antiretroviral medication to treat her HIV infection.
That presented a hazard to her own health, and perhaps to everyone else’s as well. The clinic sent Ms. Mathe up a hill, down a tight path, and back on the medication.
Ms. Mathe is part of a countrywide door-to-door nagging campaign. It’s part of a comprehensive South African attempt to halt the spread of novel coronavirus strains like the Omicron type discovered here last week.
The other half is at a cutting-edge facility 25 miles away. Thousands of coronavirus genomes are sequenced each week at the KwaZulu-Natal Research Innovation and Sequencing Platform in Durban. With decades of experience fighting H.I.V., the KRISP lab found both the Beta and Omicron forms.
Combining sophisticated tech and grassroots activism, this is a frontline fight against the developing coronavirus. On Friday, the South African research network announced to a world eager for news that the new variety looked to spread twice as fast as Delta, the virus’s most infectious strain.
KRISP researchers are world pioneers in viral phylogenetics, the study of virus evolution. In order to stop the spread of the coronavirus, researchers examine changes in the virus across samples and identify transmission hotspots.
They have been monitoring the virus’s alterations in South Africa since the epidemic began because they are concerned about the eight million individuals living with HIV (13% of the population).
When HIV patients take an effective antiretroviral regularly, their systems virtually entirely suppress the virus. HIV impairs the immune systems of individuals who aren’t diagnosed, aren’t treated, or can’t take their medications regularly. A coronavirus infection might take weeks or months to remove from the body.
When the coronavirus stays in their systems for so long, it has the ability to evolve. And if they spread the altered virus, a new strain emerges.
“We suspect that some of the developing variations in South Africa might be directly linked to HIV,” said Tulio de Oliveira, lead investigator of the national genetic surveillance network.
A COVID death is 1.7 times more likely if you have HIV than if you have diabetes, which is 30 times more likely. “Once we recognised this, we realised that critically immunocompromised persons might lead to new variants,” Dr. Abdool Karim added.
KRISP researchers found evidence of this happening twice. An H.I.V. patient who was not being helped to discover treatments she could tolerate was linked to a viral sample last year. During that period, the viruses mutated 32 times within her body.
Doctor de Oliveira and his team tracked a coronavirus sample with hundreds of mutations to the Western Cape in November, where another patient was apparently failing to take his HIV drugs. The coronavirus persisted in her body for months, mutating her. When these ladies were given efficient medications and instructed on how to use them, they swiftly recovered.